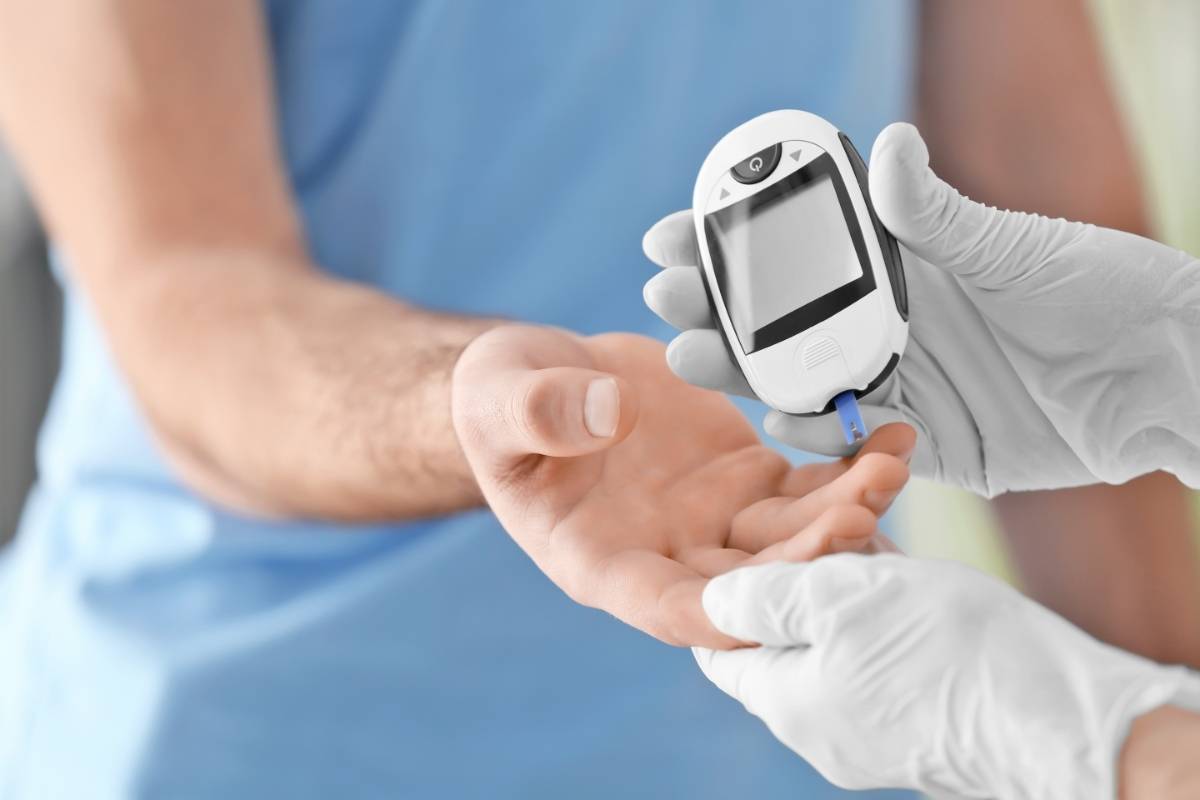
The 5 Biggest Myths About Diabetes Programs (And What Actually Works)
You've been told to "manage your diabetes." Eat better. Move more. Check your blood sugar. But when you search for a Diabetes Program, you're flooded with options. Apps that promise to reverse diabetes in 8 weeks. Coaches who charge $500 a month. Support groups that meet at inconvenient times. It's overwhelming. And most of it doesn't work for real people with real lives.
This guide cuts through the noise. We'll bust the five most common myths about diabetes programs, show you what actually moves the needle on your A1C, and help you build a plan that fits your budget, your schedule, and your specific type of diabetes.
Part 1: Myth #1 – "You Need an Expensive, High-Tech Program to See Results"
Walk into any diabetes-focused marketing funnel and you'll see the same promises: AI-powered coaching, continuous glucose monitors (CGMs) for everyone, personalized meal plans delivered daily. The price tag? $200 to $500 per month.
The truth: Most of the A1C improvement in any diabetes program comes from three cheap (or free) interventions.
What actually works:
Walking after meals. A 10-minute walk after dinner lowers blood sugar by 20-30 mg/dL. Cost: $0.
Consistent carb intake. Eating roughly the same amount of carbs at the same meals each day makes medication dosing predictable. Cost: $0.
Taking metformin as prescribed. Metformin costs $4-$30 per month. It's the most studied, safest oral diabetes medication. Yet studies show nearly 30% of people prescribed metformin aren't taking it consistently.
Before you pay for a high-tech program: Try these three things for 30 days. Track your fasting blood sugar. Most people see a 10-20 point drop without spending a dime.
Part 2: Myth #2 – "A Diabetes Program Is Only for People With Type 2"
Search for Diabetes Program and most results assume you have Type 2. Weight loss tips. Lifestyle coaching. "Reverse your diabetes" promises. If you have Type 1, none of this applies to you.
The truth: Type 1 diabetes requires a completely different program focus.
What a Type 1 diabetes program should include:
Carb counting training (not just "eat less carbs" – exact gram counting)
Insulin adjustment protocols (how to change your basal and bolus based on CGM trends)
Sick day rules (when to increase insulin, when to check ketones)
Hypoglycemia management (how to treat lows without over-correcting)
Where to find it: Look for programs affiliated with academic medical centers (Mayo Clinic, Johns Hopkins, Joslin Diabetes Center). Avoid generic "diabetes reversal" programs – they're not designed for Type 1.
| Program Feature | Type 2 Focus | Type 1 Focus |
|---|---|---|
| Weight loss | Central (often leads to remission) | Helpful but not primary |
| Carb counting | General ("choose whole grains") | Exact gram counting |
| Insulin management | Adding or adjusting | Fine-tuning basal/bolus ratios |
| Hypoglycemia | Rare (except on sulfonylureas) | Daily concern |
Part 3: Myth #3 – "You Need a CGM to Be Successful"
Continuous glucose monitors (CGMs) are amazing tools. They show you real-time blood sugar trends. They alert you to dangerous lows. They've transformed Type 1 management.
The truth: For many people with Type 2 not on insulin, a CGM is nice to have – but not necessary for good control. Studies show that structured self-monitoring with a $20 glucometer can achieve similar A1C improvements as CGM, if you actually use the data.
When you actually need a CGM:
You have Type 1 diabetes (standard of care)
You take insulin and have frequent lows (especially overnight)
You've tried fingerstick monitoring but your A1C remains above 9%
When you can skip the CGM:
You have Type 2 not on insulin
You check fasting blood sugar regularly and it's in range
Your A1C is below 7.5%
The cheaper alternative: A basic glucometer ($10-20) and test strips ($9-18 for 50). Check fasting and 2 hours after your largest meal. That's 2 strips per day. $15-30 per month. Compare that to CGM sensors at $300-500 per month without insurance.
Part 4: Myth #4 – "The Best Diabetes Program Is the One Your Doctor Recommends"
Your doctor means well. But most primary care physicians don't have time to vet every diabetes app, coaching service, or support group. They'll recommend whatever the drug rep left on their desk or whatever the hospital system is affiliated with.
The truth: The best Diabetes Program is the one you'll actually use. A gold-standard program that you hate and avoid is worthless. A mediocre program that you engage with daily will improve your health.
How to choose a program that fits your life:
Time commitment. Can you do 2 hours per week? 30 minutes per week? Be honest.
Format. Do you prefer in-person groups, one-on-one coaching, or self-guided app?
Cost. What's your budget? Many Medicare-eligible programs are free. Commercial programs range from $50-$500/month.
Technology comfort. Do you want a CGM and app? Or do you prefer paper logs and phone calls?
Red flags to avoid:
Programs that guarantee diabetes "reversal" in a fixed time (8 weeks, 12 weeks)
Programs that require expensive supplements or proprietary foods
Programs that discourage you from taking prescribed medications
Programs with no licensed medical professionals on staff
Part 5: Myth #5 – "Once You Start a Program, You Can Never Stop"
Diabetes programs often feel like a life sentence. Weekly check-ins. Daily logging. Constant reminders that you have a chronic condition. It's exhausting.
The truth: A good Diabetes Program should teach you skills, not just provide services. The goal is to eventually need less support, not more.
What skills you should gain in the first 6 months:
How to adjust your own medication (with doctor supervision)
How to respond to high and low blood sugar without panic
How to eat at restaurants, parties, and holidays without spiking
How to exercise safely without crashing
Signs you're ready to "graduate" from formal programs:
Your A1C has been stable for 6 months
You haven't had a severe low in the past year
You can troubleshoot high blood sugar without calling your coach
You have a support system (family, friends, online group) outside the program
Maintenance mode: After you graduate, check in with your care team every 3-6 months. Re-enroll in a program if your A1C rises by 1% or you have a major life change (new diagnosis, medication change, hospitalization).
Part 6: What a Good Diabetes Program Actually Looks Like
Now that we've busted the myths, here's what to look for in a Diabetes Program that actually works.
For prediabetes (prevention-focused):
National DPP (Diabetes Prevention Program) – 1 year, 22 sessions, covered by Medicare
Focus: 5-7% weight loss, 150 min/week physical activity
Format: In-person groups or online (Omada, Noom for Diabetes)
Cost: $0-$50 per month (many covered by insurance)
For Type 2 diabetes (management-focused):
DSMES (Diabetes Self-Management Education and Support) – 10 hours first year, covered by Medicare
Focus: Medication management, blood sugar monitoring, nutrition, sick days
Format: Usually in-person at hospitals or clinics; some virtual options
Cost: Often $0 with insurance
For Type 1 diabetes (technology-focused):
JDRF T1D Support Network – peer support, not formal education
Integrated Diabetes Services – virtual coaching for pump and CGM users
Focus: Carb counting, insulin adjustment, advanced technology
Format: One-on-one virtual coaching
Cost: $100-$300 per session (not typically covered)
| Program Type | Best For | Typical Cost | Insurance Coverage |
|---|---|---|---|
| National DPP | Prediabetes | $0-$50/month | Medicare, many private plans |
| DSMES | Type 2 (newly diagnosed) | Often $0 | Medicare, most insurance |
| Virtual coaching | Type 2 (established) | $50-$200/month | Variable |
| Endocrine specialty | Type 1 | Copay only | Most insurance |
Part 7: Your 90-Day Diabetes Program Starter Plan
No money for a formal program? No problem. Here's a 90-day plan you can do on your own.
Month 1 – Foundation
Week 1: Buy a glucometer ($10-20). Check fasting blood sugar every morning.
Week 2: Add a 10-minute walk after dinner. Track your steps.
Week 3: Log your carbs at one meal per day. Just write them down – no judgment.
Week 4: Review your fasting numbers. Have they improved? If not, focus on dinner carbs.
Month 2 – Build
Week 5: Add a second walk (10 minutes after lunch).
Week 6: Start a food log for all meals. Note how you feel 2 hours after eating.
Week 7: Identify your "spike foods" – meals that raise your blood sugar above 180. Reduce or replace them.
Week 8: Check your A1C (ask your doctor or buy a home test). Celebrate any improvement.
Month 3 – Sustain
Week 9: Join a free online support group (Facebook, Reddit's r/diabetes, TuDiabetes).
Week 10: Share your food log with a friend or family member. Accountability helps.
Week 11: Try one new diabetes-friendly recipe each week.
Week 12: Re-check A1C. Compare to baseline. Set goals for the next 90 days.
Cost of this DIY program: $20 for glucometer + $30 for test strips + $50 for home A1C tests = $100 total. That's less than one month of most commercial programs.
Part 8: Frequently Asked Questions About Diabetes Programs
Do I really need a formal diabetes program?
Not necessarily. If your A1C is below 7%, you know how to adjust your medications, and you haven't had a severe low in the past year, you may not need formal support. But programs are helpful for new diagnoses, A1C above 8%, or major life changes.
Are online diabetes programs as good as in-person?
For most people, yes. Studies show virtual diabetes programs achieve similar A1C reductions as in-person programs, with higher completion rates (people actually finish online programs). The key is engagement – whichever format you'll stick with.
What's the cheapest diabetes program?
Medicare's National DPP and DSMES are often free. For everyone else, look for hospital-based programs (sliding scale fees) or community health centers. Avoid multi-thousand-dollar "reversal" packages – they're almost never worth the cost.
Can a diabetes program help me stop taking medication?
Maybe. If you have Type 2 and lose significant weight (10-15%), some people achieve remission (normal blood sugar without medication). But any program that guarantees medication reduction should be viewed skeptically. Work with your doctor.
What if I've tried programs before and failed?
Most programs assume you fail because you lack motivation. That's usually wrong. More likely, the program didn't fit your life. Try a different format. If you failed a high-tech CGM program, try a low-tech paper log. If you failed an in-person group, try one-on-one coaching. The right fit makes all the difference.
.jpg)

.jpg)
.jpg)



