Dental Implants: A Practical Guide to Restoring Smiles
Introduction
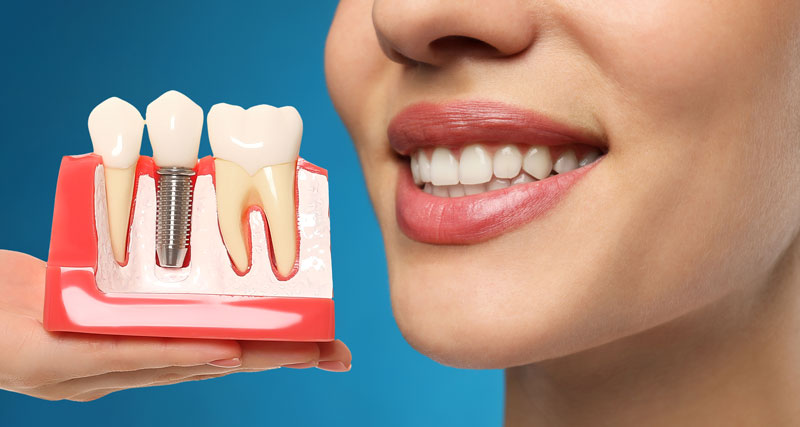
Dental implants have become a standard solution for replacing missing teeth. They provide both functional stability and aesthetic improvement, often improving chewing, speech, and self-confidence. This article explains what implants are, who is a candidate, the step-by-step process, potential risks, and how to care for implants long term.
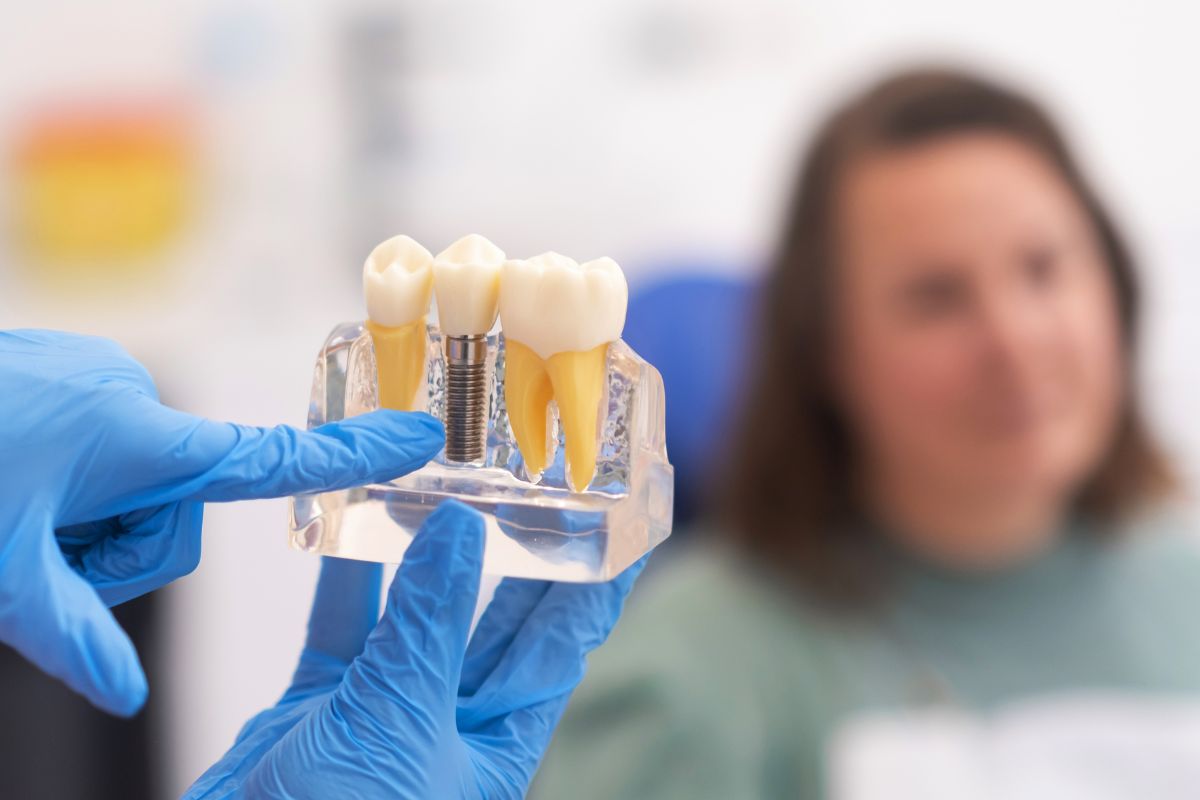
At their core, dental implants are small posts—typically made of titanium or zirconia—placed into the jawbone to serve as artificial tooth roots. Once integrated with bone, they support crowns, bridges, or dentures. Unlike removable options, implants offer a fixed foundation that behaves much like natural teeth.
Who is a good candidate?
Most adults who have lost one or more teeth can be considered for implants. Ideal candidates generally meet these criteria:
- Good overall health without uncontrolled systemic disease (e.g., uncontrolled diabetes).
- Adequate jawbone volume and density at the implant site, or the willingness to undergo bone augmentation.
- Healthy soft tissues and controlled periodontal (gum) disease.
- Commitment to oral hygiene and regular dental visits.
Certain factors may complicate implant treatment: heavy smoking, untreated periodontal disease, certain medications, or systemic conditions that impair healing. A thorough clinical and radiographic assessment helps determine candidacy and treatment planning.
Types and materials
The most common implant types are endosteal (placed within the bone) and subperiosteal (placed on top of the bone but under the gum), though endosteal implants dominate modern practice. Materials commonly used are:
- Titanium: Highly biocompatible, excellent long-term integration with bone.
- Zirconia: Metal-free alternative with good aesthetics and growing clinical evidence.
Abutments (connectors) and final restorations (crowns/bridges) come in different shapes and materials. Your dentist will choose components based on location, load demands, and aesthetic needs.
The treatment process: step by step
While protocols can vary, the implant journey typically follows these stages:
- Consultation and planning: Clinical exam, dental impressions, and 3D imaging (CBCT) to evaluate bone anatomy and plan implant position.
- Surgical placement: Under local anesthesia (with sedation if needed), the implant is placed into the bone. Sutures are used to close the site.
- Osseointegration: A healing period—usually 3 to 6 months—during which bone bonds to the implant surface. Temporary restorations may be provided.
- Abutment and restoration: Once integrated, an abutment is attached and an impression taken for the final crown, bridge, or denture.
- Maintenance: Regular follow-ups and lifelong oral hygiene support implant longevity.
In some cases, immediate loading (placing a provisional crown the same day) is possible when primary stability is sufficient. Conversely, bone grafting or sinus lifts may precede implant placement in sites with inadequate bone.
Risks and complications
Dental implants have high success rates, but complications can occur. Common issues include:
- Infection or peri-implantitis: Inflammation around the implant that can lead to bone loss if untreated.
- Implant failure: Failure to integrate with bone, sometimes requiring removal and replacement.
- Nerve or sinus injury: Rare if careful planning isn’t performed; thorough imaging reduces risk.
- Prosthetic complications: Loosened screws, fractured restorations, or wear that require repair.
Early diagnosis and intervention—improved hygiene, professional cleaning, or surgical treatment—can often manage complications effectively.
Aftercare and long-term success
Successful implants require attention after placement. Key recommendations include:
- Maintain diligent oral hygiene: brushing twice daily, interdental cleaning around implants, and using antimicrobial rinses if advised.
- Attend regular dental check-ups and professional cleanings every 3–12 months based on risk.
- Avoid tobacco and address parafunctional habits like bruxism (night guards may be recommended).
With proper care, implants can last for decades. Longevity depends on systemic health, oral hygiene, quality of the prosthesis, and regular maintenance.

Cost and alternatives
Implants typically cost more upfront than removable dentures or bridges, but their durability and function can make them cost-effective over time. Alternatives include fixed bridges (requiring adjacent tooth preparation) and removable dentures. Discuss functional needs, budget, and expectations with your dentist to find the right solution.
Final thoughts
Dental implants offer a reliable, natural-feeling way to replace missing teeth when planned and maintained properly. An experienced implant team, thorough diagnostic work, and patient commitment to oral health are the pillars of predictable outcomes. If you’re considering implants, schedule a consultation to review your options and personalized treatment plan.
"Informed decisions and careful maintenance turn modern implant dentistry into lasting, life-changing results."
If you have specific concerns—medical conditions, bone loss, or finances—bring them up early. A transparent discussion helps tailor a predictable, comfortable path to restoring your smile.
.jpg)

.jpg)
.jpg)



